Vol-1 Issue-1 Year-2026
Dr. Manisha Aluri, MD, Paediatrics, Citizens Speciality Hospital, Nallagandla, Hyderabad
Author of Correspondence: Dr. Manisha Aluri, MD, Paediatrics, Citizens Speciality Hospital, Nallagandla, Hyderabad
Email: manisha.aluri@gmail.com@gmail.com
KEYWORDS:
Lemierre syndrome, Fusobacterium necrophorum, oropharyngealinfection, acute pharyngitis, septic
thromboembolism
Received date-02-03-2026
Accepted date-17-03-2026
Published date -22-03-2026
Citation format: Aluri M. When
oropharyngeal infection turns deadly:
A case of Lemierre syndrome. J Dent
Innov Med Sci. 2026;1(1):23–25
Oropharyngeal infections are among the most common illnesses in the pediatric population. They are frequently diagnosed with viral pharyngitis and managed symptomatically, particularly when accompanied by cough, nasal congestion, and diffuse myalgias. However, findings such as prolonged fever, muffled voice, neck pain, or chest pain warrant further evaluation to exclude serious complications, including peritonsillar abscess, meningitis, and pneumonia. A rare but life-threatening complication of acute bacterial pharyngitis is Lemierre syndrome (LS), a necrotizing oropharyngeal infection most commonly caused by Fusobacterium necrophorum (F. necrophorum), an anaerobic organism that can progress to septic thrombophlebitis and thromboembolism involving the systemic and pulmonary circulation. This is a case of LS initially suspected to be pharyngitis with peritonsillar abscess that subsequently progressed to pulmonary septic thromboembolism.
Introduction
Lemierre syndrome is a virulent disease involving septic thrombophlebitis of the internal jugular vein (IJV) in association with systemic/pulmonary thromboembolism, following a recent history of oropharyngeal infection [1]. It occurs in otherwise healthy adolescents or young adults [2-4]. It is one of the rarest complications of an oropharyngeal bacterial infection, most caused by an obligate anaerobic bacterium, F. necrophorum. Diagnosis requires a high index of suspicion, especially if the clinical course deviates from the normal progression of an oropharyngeal infection. Prompt treatment is warranted to prevent fatal complications such as sepsis, end organ damage and death.
Case Report
A fully vaccinated 14-year-old male with no significant past medical history presented to the emergency department with 4 days of high-grade fever and 6 days of severe sore throat, voice change, cough, and dysphagia. On presentation, he was febrile to 102.4 °F and tachycardic to 113 beats/min, with normal blood pressure, oxygen saturation, and respiratory rate.
Physical examination revealed a distressed adolescent with left-sided neck swelling and restricted neck movement secondary to pain. Cardiopulmonary and abdominal examinations were unremarkable. He was alert and oriented to time, place, and person.
Given concern for peritonsillar abscess with possible sepsis, laboratory workup was initiated, and the patient was started on intravenous fluids, analgesics, and empiric piperacillin–tazobactam for broad-spectrum anaerobic coverage. Neck radiography supported the diagnosis of peritonsillar abscess. He was admitted for continued intravenous antibiotic therapy pending blood culture results.
Overnight, he developed worsening cough, hemoptysis, dyspnea, and hypoxia requiring supplemental oxygen, prompting transfer to the intensive care unit. Chest radiography demonstrated bilateral lower lobe patchy infiltrates and nodules. Computed tomography of the chest and neck revealed IJV thrombosis and bilateral pulmonary emboli consistent with septic emboli, raising suspicion for LS. Blood cultures obtained on admission subsequently grew F. necrophorum, confirming the diagnosis.
The patient continued on intravenous piperacillin–tazobactam. His respiratory status improved significantly over 5 days with supportive care, including noninvasive ventilation. He completed a total of 6 weeks of intravenous antibiotic therapy with full clinical recovery.
Discussion
Lemierre syndrome is a life-threatening bacterial infection of the parapharyngeal space caused by F. necrophorum. It is a gram-negative bacillus and a part of the normal flora in the oropharyngeal and gastrointestinal tract in pediatric patients. F. necrophorum may be present in the throat swabs of up to 21% of healthy individuals [1]. LS primarily occurs in young, otherwise healthy adolescents, and predominantly in males [2,3,4]. As an obligate anaerobe, the bacterium thrives well in the peritonsillar abscess, allowing it to penetrate the adjacent tissues. Extension of the infection from the oropharynx into the lateral pharyngeal space results in the seeding of the IJV, septic thrombophlebitis, and subsequent access to the venous system, resulting in septicemia and septic emboli [2]. One hypothesis states that organisms like Epstein-Barr Virus (EBV) cause local mucosal damage and inflammation, thereby assisting F. necrophorum to invade surrounding tissues [1].
LS has a prodrome of acute pharyngitis, complicated by a worsening clinical course due to the onset of systemic and pulmonary septic thromboembolism. Patients present with symptoms associated with systemic septic thromboembolism. Most frequently affected organ is the lungs (85%), although joints, liver, kidney, brain, bones, heart, and meninges can all be involved [2].
LS is a clinical diagnosis. Blood culture is the gold standard, although it may be negative in upto 30% of cases [2]. Other haematological investigations are recommended to evaluate end organ function, such as leukocytosis and thrombocytopenia, hepatic transaminitis, and elevated creatinine. A chest X ray may demonstrate patchy infiltrates if there are pulmonary septic emboli. IJV thrombophlebitis may be diagnosed using an ultrasound Doppler. CT scan of the chest and neck is widely used to evaluate for the IJV thrombosis and pulmonary septic emboli (Fig 1&2). The main stay of treatment is broad spectrum antibiotics like beta lactamase resistant penicillin, and clindamycin with significant anaerobic coverage. Additionally, supportive care (intravenous fluids, ventilation assistance for pulmonary insufficiency and dialysis for renal impairment) is the cornerstone of management when systemic or pulmonary septic emboli are identified. Anticoagulation is a controversial discussion, but in general, indicated if there is involvement of cerebral venous sinuses [1]. LS may also require surgical intervention as part of the management of metastatic septic lesions. This may include procedures such as IJV ligation, pleural drainage, abscess drainage, mastoidectomy, tonsillectomy, and invasive cranial surgery [1]. On appropriate antibiotic therapy, infection to defervescence takes about a week. Prolonged course of about 4-6 weeks of IV antibiotics is recommended for complete resolution [5].
Prognosis was unfavorable in the pre-antibiotic era. After the introduction of beta lactamase resistant antibiotics, the mortality has significantly reduced, albeit, with appropriate antibiotics and therapy, mortality has been reported to be between 5% and 18% [2]. If left undiagnosed or untreated, LS is fatal.
Conclusion
Most cases of pharyngitis in the pediatric population are viral in etiology and are usually self-limiting without any complications. Presence of atypical symptoms/prolonged or worsening symptoms, warrant a detailed evaluation to exclude the possibilities of coexisting bacterial infections, of which LS is one of the grave forms. It leads to systemic thrombophlebitis and thromboembolism and can be fatal. Therefore, a high index of suspicion is required to ensure timely recognition and appropriate management.
Funding Source: No funding was secured for this case report.
Financial Disclosure: The authors have no financial relationships relevant to this article to disclose.
Conflict of Interest: none
Clinical Trial Registration: Not applicable.
References
1.Tiwari A. Lemierre’s Syndrome in the 21st Century: A Literature Review. Cureus. 2023 Aug 18;15(8):e43685.
2.Allen BW, Anjum F, Bentley TP. Lemierre Syndrome. 2023 Jul 31. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan.
3.Foo EC, Tanti M, Cliffe H, Randall M. Lemierre’s syndrome. Pract Neurol. 2021 Oct;21(5):442-444.
4.Kliegman, R. M., & St. Geme, J. W. (Eds.). (2024). Nelson Textbook of Pediatrics (22nd ed.). Elsevier.
5.Johannesen KM, Bodtger U. Lemierre’s syndrome: current perspectives on diagnosis and management. Infect Drug Resist. 2016 Sep 14;9:221-227.
Figures
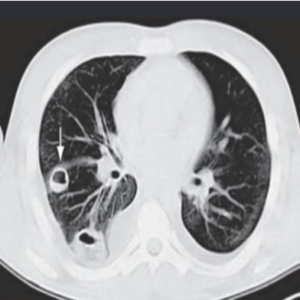
Fig 1: CT chest demonstrating nodular pulmonary infiltrates, suggesting metastatic pulmonary abscess in patient with LS.
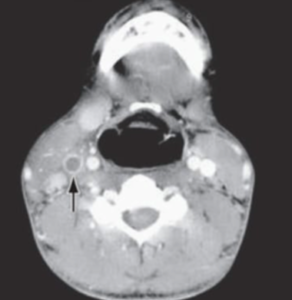
Fig 2: CT neck demonstrating the right IJV thrombus


